(see also: Pyknodyostosis)
Discussion:
- disease characterized by failure of maturation and organization of collagen fibers;
- defect in collagen (procollagen to type I collagen sequence and abnormal cross linking) leading to decreased collagen secretion,
bone fragility;
- there may be an inability to form normal bone due to a defect in osteoblastic function;
- with the formation of abnormal bone, there is a secondary, though not precisely understood, increase in resorption of bone with a
secondary increase in bone turnover;
- osteoid mineralization, osteoclastic activity, and intramembranous bone formation are not affected;
- classification of osteogenesis imperfecta:
- note that there is a wide variety in the OI phenotype, but all share in osseous fragility and propensity for fracture;
- diff dx:
- juvenile osteoporosis
- rickets
- battered child syndrome
- leukemia;
- abundant frx callus may be mistaken for osteosarcoma;
- references:
- Distinct biochemical phenotypes predict clinical severity in nonlethal variants of osteogenesis imperfecta.
- Studies of collagen synthesis and structure in the differentiation of child abuse from osteogenesis imperfecta.
- Clinical Features:
- short stature, scoliosis, tooth defects, hearing defects, propensity for fractures, and ligamentous laxity;
- other abnormalities associated with abnormal collagen formation are evident, such as blue sclerae, abnormalities of tooth
formation and skull shape, and occasional deafness;
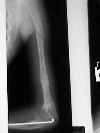
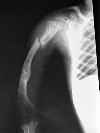
- fractures:
- results from marked loss of bone and leads to significant lack of growth of bone in length, and multiple deformities secondary
to these fractures;
- femur fractures are most common but tibial frx may show most severe angulation;
- frxs may occur at any age, but frx occurance frequently decreases as age increases (often fractures cease at puberty);
- some adults affected with this disorder will only give a history of occassional fractures and mild osteopenia;
- fractures tend to heal readily w/ exuberant callus, but the callus formed is of poor quality (identical in structure with the rest of
the skeleton);
- hence it is easily deformed by forces associated with wt bearing;
- ref: Fractures at Diagnosis in Infants and Children With Osteogenesis Imperfecta
- joints:
- laxity of the ligaments results in hypermobile joints & increased incidence in joint dislocation;
- hearing:
- hearing defects 2nd to inner and middle ear abnormalities may develop, & affected children require regular audiologic
examinations;
- pelvis:
- protrusio acetabuli may occur in type III and may narrow pelvic outlet, and can cause constipation or even partial obstruction of
rectosigmoid colon;
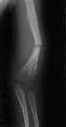
- Radiographs:
- bones are gracile and diffusely osteopenic, w/ thin cortices & attenuated trabecular pattern;
- note that w/ some OI phenotypes, radiographic osteopenia may be slight and may be missed on x-ray; (in these cases, consider
dual energy x-ray absorptiometry);
- references:
- The role of dual energy x-ray absorptiometry in aiding the diagnosis of pediatric osteogenesis imperfecta.
- Treatment:
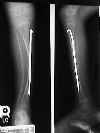
- Sofield osteotomy:
- indicated for OI patients w/ repetitive frx or progressive angular deformity in a weightbearing bone;
- involves multiple realignment osteotomies and internal fixation with a load sharing IM device is the treatment of choice;
- reference:
- The Sofield-Millar operation in osteogenesis imperfecta A modified technique.
- bone grafting is not required for fracture healing, and compression plating predisposes to further fracture;
- bone deformities caused by microfrx on tension side are common;
- when severe enough to interfere with bracing or allow recurrent frx, multiple realignment osteotomies (Sofield), fixed w/
expandable IM rods is performed;
- note that these patients may be at risk for malignant hyperthermia;
- all substantial deformities should be corrected simultaneously to limit immobilization time;
- postop bracing to avoid recurrent deformity must be considered;
- Spine:
- cervical spine:
- basilar impression may occur in up to 25% of patients (more common w/ type IV);
- MRI is radiographic study of choice;
- thoraco-lumbar spine:
- scoliosis develops in over 50% of involved patients;
- bracing is ineffective because of the plasticity of the chest wall;
- surgical correction w/ posterior instrumentation is usually successful;
- bone fragility may complicate surgical fixation;
- hooks may be reinforced with methylmethacrylate;
- segmental instrumentation techniques have been used successfully;
- vertebral compression of fractures caused by osteoporosis can occur at any age and may lead to symptomatic back deformities;
- references:
- The operative management of basilar impression in osteogenesis imperfecta.
- The spine in osteogenesis imperfecta.
- Osteogenesis imperfecta. Radiographic classification, natural history, and treatment of spinal deformities.
References
Non-union of fractures in children who have osteogenesis imperfecta.
Aftermath of osteogenesis imperfecta: the disease in adulthood.
Hip and knee replacement in osteogenesis imperfecta.
Microvascular and cellular defects of the periosteum of osteogenesis imperfecta.
Gastrointestinal problems in patients who have type-III osteogenesis imperfecta.
Fractures in childhood: osteogenesis imperfecta or child abuse?
Functional Significance of Bone Density Measurements in Children with Osteogenesis Imperfecta.
Deficiency of Cartilage-Associated Protein in Recessive Lethal Osteogenesis Imperfecta.