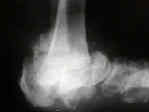
 - See: diabetic foot menu
- See: diabetic foot menu
- Diabetic Charcot Foot and Ankle:
- originally described in the 1860s by the neurologist Jean-Martin Charcot;
- may occur w or w/o neuropathic ulceration (mal perforant):
- typically appears in 5th and 6th decades;
- often occurs in the face of a relatively "normal vascular exam;"
- neuropathic ulcerations are common with charcot arthropathy even in the absence of protective sensation;
- below knee amputation is usually avoidable in the Charcot foot;
- inciting factors:
- peripheral neuropathy
- unrecognized injury
- continued repetitive stress on injured structures
- increased local blood flow;
- excessive osteoclastic activity w/o a concomitant increase in osteoblastic function;
- pathoanatomy:
- includes cartilaginous fibrillation and destruction and subchondral/enchondral bone formation;
- charcot joint can result in fragmentation of periarticular areas & subluxations:
- usually affects midtarsal joints and can lead to prolapse of the arch or valgus deviation of the forefoot;
- reference:
Cytokine-induced osteoclastic bone resorption in charcot arthropathy: an immunohistochemical study.
- natural history: (see radiographic stages below)
- early (stage 1) neuroarthropathy:
- hyperemia, warmth, and swelling;
- late (stage 3) neuroarthropathy
- after the initial presentation, there will be less edema and warmth;
- bone consolidation occurs, and foot may develop loss of arch and rocker bottom deformity;
- radiographs may show neuropathic changes w/ fractures, dislocation of of joints, and bony disintegration;
- reference:
- Radiographic and clinical classification of acquired midtarsus deformities.
- Progression of Foot Deformity in Charcot Neuropathic Osteoarthropathy
- Clinical Features:
- initial presentation:
- may resemble osteomyelitis in that foot appears swollen with overlying erythema and warmth;
- history, exam, laboratory data, and radiographs can all help to distinguish between Charcot joint and infection;
- exam:
- w/ neuropathic foot, pt may present with a hot swollen erythematous, but painless foot;
- elevation of the foot for 1-2 hours should eliminate erythema and swelling w/ neuropathic foot but not infection;
- note that these clinical symptoms do not correlate with radiographic staging;
- pt w/ dense neuropathy will have marked muscle wasting which should not be confused with ischemia;
- skin can be tested w/ a Semmes-Weinstein monofilament (sensation w/ the 5.07 filament indicates protective sensation);
- if ulceration is present, it will be of the mal perforant type vs the ischemic type;
- an ulcer that leads directly down to bone (along w/ radiographic osteolytic changes) is more indicative of infection;
- labs: w/ Charcot foot
- glucose under control and the HA1c is normal;
- normal ESR
- neurological exam
- in exam of the diabetic foot note the neurologic findings are usually distal, symmetrical, and sensory;
- absent or diminished tendon reflexes are characteristic findings;
- ankle jerk is mainly affected and is absent 4 times > knee jerk;
- diminution or loss of vibratory sense in the area of the foot and ankle is also common;
- development of claw toes occurs as a result of peripheral neuropathy w/ loss of foot instrinsics;
- clawing of toes may result in anterior displacement of the forefoot fat pad leading to metatarsalgia;
- in trying to distinguish between a neuropathic foot and an infection, consider observing the foot after it has been elevated for 5 min;
- peristence of erythemia is more consisent with infection (and vice versa, disappearance of erythema is consistent with a Charcot foot);
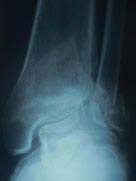
- Radiographs and Natural History:
- early changes:
- may present as a low energy fracture with joint subluxation and dislocation;
- bone fragmentation and erosions may be seen in early stages;
- wt bearing radiographs help accentuate joint subluxation if it present;
- mid stage changes:
- resorption and coalescence of fragments (large fragments may fuse together);
- bone surrounding the joint becomes sclerotic
- absorption of the fine debris occurs
- bone and joint stability increases and the deformity ceases to rapidly progress
- late changes:
- reconstruction and reconstitution phase;
- osteolysis may be present w/ both Charcot joints and osteomyelitis;
- hypertrophic changes can accompany joint destruction;
- remodeling occurs with reduction of the sclerosis;
- there is rounding of the major fragments;
- there is an attempt at reformation of the joint architecture w/ stabilization and near ankylosis;
- bone scanning (gallium scan or indium scan) may help to r/o osteomyelitis, but these are usually not necessary;
- reference:
- Diabetic neuropathy in the foot: patient characteristics and patterns of radiographic change.
- Management:
- goals of treatment are generally to avoid osseous prominences (which can lead to ulnceration) and to restore foot stability;
- prevention of plantar ulceration: (see: neuropathic ulceration)
- bisphosfonates: (fosamax)
- there is early evidence that the destructive changes in neuropathic arthropathy may be mediated by osteoclasts and may be tempered by bisphosfonates;
- reference:
- Bisphosphonates in the treatment of Charcot neuroarthropathy: a double-blind randomised controlled trial.
- immobilization and off loading:
- in early and mid stages, the patient needs to stay off the affected foot (which is difficult when there are bilateral charcot changes;
- custom foot wear or patellar tendon bearing / custom clam shell orthosis (either for short term use in early disease or for severe deformities);
- casting prevents patients from cheating and removing the orthosis;
- total contact casting helps distribute wt bearing forces more evenly than regular casts;
- when a patient presents w/ a low energy Charcot fracture non-wt bearing immobilization for an extended period of time is necessary;
- w/ either midfoot or ankle neuropathic changes, prolong immobilization is usually necessary (often 1-2 years), until foot stability returns;
- if skin ulcers over a midfoot exostosis cannot be managed with shoe/orthotic modifications then surgical excision of the exostosis
is indicated (do not turn a stable midfoot into an unstable midfoot);
- references:
- Charcot Arthropathy and Immobilization in a Weight-Bearing Total Contact Cast
- Patellar tendon-bearing, patten-bottom caliper suspension orthosis in active Charcot arthropathy: crutch-free ambulation with no weight bearing in the foot.
- Surgical versus accommodative treatment for charcot arthropathy of the midfoot.
- Off-loading the diabetic foot wound: a randomized clinical trial.
- treatment pitfalls and neuropathic fractures:
- need to discern between stable and unstable feet (even if foot is alignment has collapsed and is non anatomic);
- in some cases, a diabetic will sustain what appears to be a traumatic frx (such as an ankle frx), but later it is found that the fracture
occurred as a part of Charcot pathology;
- the patient should be warned that a Charcot fracture will not respond to treatment (surgical or non surgical) as well as a traumatic frx;
- in general, surgical fixation should be avoided during the early fragmentation stage of the process (rather wait for the consolidation phase);
- if surgery is necessary, keep full thickness incisions and do not attempt to avoid cutting cutaneous nerves since the foot is often already insensate;
- often surgical fixation includes joint arthrodesis, and it is of paramount importance to achieve secure hardware fixation even if it
means have screws engage an adjacent stable part of the foot;
- references:
- Fractures associated with neuropathic arthropathy in adults who have juvenile-onset diabetes.
- The management of neuropathic fracture dislocations in the diabetic patient.
- tendon transfers:
- ref: Chronic diabetic ulcers under the first metatarsal head treated by staged tendon balancing: a prospective cohort study.
- Arthrodesis and Reconstruction:
- w/ significant collapse, joints which demonstrate ligamentous instability or destructive changes on wt bearing radiographs should
be considered for arthrodesis;
- hindfoot valgus collapse: tibio talar calcaneal arthrodesis
- midfoot Charcot:
- note that there is a high infection rate (25%) when arthrodesis is performed with an open plantar ulcer;
- w/ midfoot collapse, reduction is often carried out by bone resection in addition to soft tissue release;
- Marks RM et al (1998), a plate applied to plantar (tension side) of medial forefoot gives sturdier fixation than screw fixation constructs;
- Simon, et al (2000), the authors studied the use of arthrodesis of the tarsal-metatarsal area for the treatment of Eichenholtz
stage-I Charcot arthropathy in patients with diabetes;
- 14 patients underwent ORIF and bone grafting to the TMT region;
- all patients had a successful fusion and there were no long term complications;
- early arthrodesis for Eichenholtz stage-I Charcot arthropathy of the foot noting liklihood anatomical reduction,
clinical union, and stability w/o increased risk of complications.
- references:
- Arthrodesis as an Early Alternative to Nonoperative Management of Charcot Arthropathy of Diabetic Foot.
- Midfoot fusion technique for neuropathic feet: biomechanical analysis and rationale.
- Midtarsal Arthrodesis in the Treatment of Charcot Midfoot Arthropathy
- Midtarsal Arthrodesis in the Treatment of Charcot Midfoot Arthropathy. Surgical Technique
- Arthrodesis of the diabetic neuropathic ankle joint.
- Talonavicular dislocations and midfoot arthropathy in neuropathic diabetic feet. Natural course and principles of treatment.
- Exostectomy for symptomatic bony prominences in diabetic Charcot feet.
- Realignment and Extended Fusion with Use of a Medial Column Screw for Midfoot Deformities Secondary to Diabetic Neuropathy
- Progression of Foot Deformity in Charcot Neuropathic Osteoarthropathy
- The medial column Synthes Midfoot Fusion Bolt is associated with unacceptable rates of failure in corrective fusion for Charcot
deformity. Results from a consecutive case series
- references:
- Deformity following fracture in diabetic neuropathic osteoarthropathy. Operative management of adults who have type-I diabetes.
- Salvage, with arthrodesis, in intractable diabetic neuropathic arthropathy of the foot and ankle.
- Surgical treatment of neuropathic foot deformity
On arthropathies of cerebral or spinal origin.
Management of neuropathic fractures in the foot and ankle.
Effects of desipramine, amitriptyline, and fluoxetine on pain in diabetic neuropathy.
Related Products
Roll-A-Bout
An alternative to crutches and wheelchairs. The Roll-A-Bout fully supports the lower leg guaranteeing 100% non-weight-bearing.

