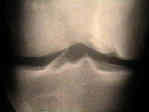
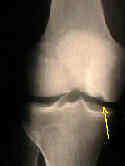
- See: Knee Joint Menu 
- Discussion:
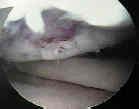
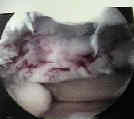
- articular cartilage injury and potential for repair;
- rotational forces in direct trauma is the most common cause of injury to the articular cartilage;
- in adults, the tidemark zone is the weak link between the overlying cartilage and subchondral
bone and therefore shearing injuries most often produce a chondral injury rather than an
osteochondral injury;
- injury is mostly in wt bearing regions of articular cartilage, and usually in medial compartment
(4 times more common that lateral injuries);
- classification
- pediatric OCD: steochondritis dessicans
- natural history:
- references:
- Isolated Full Thickness Chondral Injuries. Prevalance and Outcome of Treatment. A Study of 5233 Knee Arthroscopies.
- Articular cartilage defects: study of 25,124 knee arthroscopies
- Articular cartilage lesions in 993 consecutive knee arthroscopies
- Exam:
- symptoms of intermittent locking, recurrent effusions, crepitus, and persistant pain may all be associated with chondral injuries;
- however, similar symptoms are found in extensor mech injuries; and meniscal injuries
- with knee flexion, the anterior and central face of the medial femoral can be palpated (as opposed to the posteromedial joint
line which indicates a meniscal tear);
- w/ a dashboard type injury, consider PCL tear;
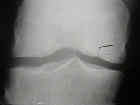
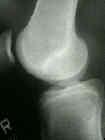
- Radiographs:
- The accuracy of magnetic resonance imaging scanning and its influence on management decisions in knee surgery.
- Sensitivity of routine 1.0-Tesla magnetic resonance imaging versus arthroscopy as gold standard in fresh traumatic chondral lesions of the knee in young adults.
- Diagnosis of chondral lesions of the knee joint: can MRI replace arthroscopy? A prospective study
- Evaluation of cartilage defects in the knee: validity of clinical, magnetic-resonance-imaging and radiological findings compared with arthroscopy
- Non Operative Treatment:
- articular steroid injection
- anti-inflammatories
- valgus unloading knee brace;
- Surgical Treatment Options:
- debridement of chondral defects and microfracture
- mosaicplasty and cartilage transplants for chrondral injuries:
- enhanced microfracture with autolgous hamstring resurfacing;
- role of allografts in repairing chondral defects: (see allografts);
- growth factors: (see BMP)
- as noted by Sellers, et al (1997), treatment with rhBMP-2 significantly accelerated formation of new subchondral bone and
improve the microscopic appearance of overlying articular cartilage;
- technical involved insertion of a BMP laden collagen sponge into a chondral defect;
- disadvantages: there may be a lack of integration of the repair tissue with the normal adjacent cartilage;
- references:
- The repair of osteochondral defects using an exogenous fibrin clot. An experimental study in dogs.
- The effect of recombinant human bone morphogenetic protein-2 (rhBMP-2) on the healing of full-thickness defects of articular cartilage. (see osteoarthritis)
Management of Articular Cartilage Injuries in the Knee (power point slide show)
Isolated chondral fractures of the knee.
Mesenchymal cell-based repair of large, full-thickness defects of articular cartilage.
Restoration of injured or degenerated articular cartilage.
Spontaneous repair of superficial defects in articular cartilage in a fetal lamb model.
Autologous chondrocyte implantation compared with microfracture in the knee. A randomized trial.
An Analysis of the Quality of Cartilage Repair Studies.
Analysis of Stored Osteochondral Allografts at the Time of Surgical Implantation.
Alternatives to Total Knee Replacement: Autologous Hamstring Resurfacing Arthroplasty