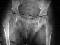
- See: cerebral palsy
- Discussion:
- may occur in upto 30% of patients w/ spastic CP, and may occur in upto 50% of patients w/ spastic quadriparetic CP;
- more severe contractures with unilateral or bilateral hip dislocation occur in the nonambulatory child with spastic quadriplegia;
- hip subluxation may be more likely in asymmetric in spastic quadriplegia and w/ pelvic obliquity and scoliosis;
- spastic deformities are initially the result of muscle tone alone;
- degree of muscle tone is difficult to quantitate, as it varies with position of adjacent joints and body posture;
- hips usually dislocate posteriorly, due to the overactivity of the adductors and flexors of hip;
- hip on the high side of the pelvis is usually dislocated, adducted, & internally rotated, whereas hip on the opposite side is located, abducted, and externally rotated;
- natural history:
- most often, the hip dislocates when the child is between 5 - 7 years of age, taking approximately two years from first evidence of subluxation;
- often the first clinical indication of subluxation is heralded by inability to abduct more than 45 deg;
- untreated dislocations may produce pelvic obliquity, pain, and problems w/ seating, decubiti, and hygiene problems;
- in the report by Knapp Jr R and Cortes H, the authors evaluate the problems associated with hip dislocation in adults with cerebral palsy;
- 29 subjects with dislocated hips and no prior hip surgery were identified;
- there were a total of 38 dislocated hips;
- age range was 21 to 52 years (average 34);
- 7 dislocated hips (18%) were definitely painful and four hips (11%) produced only mild or intermittent pain;
- 27 hips (71%) were not painful;
- 7 painful hips underwent proximal femoral resection, resulting in excellent range of motion and no pain;
- authors conclude that if a dislocated hip becomes painful in adulthood or develops an adduction contracture interfering with perineal care, a
proximal femoral resection can be performed with reliably good success;
- ref: Untreated hip dislocation in cerebral palsy
- Examination:
- check hip abduction in both extension and flexion (less than 45 deg indicates contracture, and less than 30 deg abduction indicates a significant contracture);
- Treatment:
- usually requires both a bony and a soft tissue procedure;
- both hips are done with soft tissue procedures;
- for child with spastic diplegia, adductor tenotomy or posterior transfer, with iliopsoas lengthening when the
adduction deformity is accompanied by flexion contracture, typically is done between 4 and 9 years of age;
- Early Treatment: (w/ > 40% subluxation);
- flexion and adduction contractures:
- soft tissue releases may be effective if performed before significant dysplasia is present;
- soft tissue releases should not be expected to improve osseous deformity;
- spastic deformities can result in fixed contractures that can progress to fixed joint contractures;
- contracture of psoas muscle is cause of flexion deformity in spastic diplegia as well as in spastic quadriplegia;
- treatment:
- soft tissue releases w/ post operative abduction bracing may prevent dislocation when performed before femoral head is 50% uncovered;
- iliopsoas procedures:
- poas lengthening (resection) may be indicated with hip flexor contracture (positive Thompson test)
- preservation of the iliacus maintains the strength of hip flexors;
- appreciable weakness of flexion of hip occurrs after iliopsoas tenotomy, and therefore avoid this procedure in patients who can walk;
- bilateral adductor tenotomy;
- beaware, unilateral soft-tissue surgery may have negative effect on opposite hip;
- w/ bilateral hip flexion contractures, unilateral soft tissue release may cause the contralateral hip to undergo progressive subluxation;
- hip that continues to subluxate after adductor release may require pelvic or femoral procedure and should be watched closely;
- references:
- Soft-Tissue Releases to Treat Spastic Hip Subluxation in Children with Cerebral Palsy.
- Treatment in Older Children w/ CP:
- varus femoral osteotomies;
- this may correct femoral valgus and anteversion abnormalities, but will not be expected to correct acetabular dsyplasia;
- neck shaft angle of more than 145 deg is an indication for trochanteric osteotomy, with a goal of reducing the neck shaft angle to less than 125 deg;
- derotational osteotomy may produce more normal gait but does not necessarily increase stride length;
- this operation can be done at the supracondylar level, but if there is significant valgus or subluxation of the hip, it should be done in intertrochanteric region;
- salter osteotmy;
- may have better success in DDH rather than spastic dislocation;
- chiari osteotomy;
- some authors feel that this osteotomy is contra-indicated w/ spastic dislocation;
- pemberton pericapsular osteotomy:
- indicated for acetabular dysplasia, subluxation, and dislocation;
- may not provide optimal posterior coverage;
- spastic dislocation:
- acute dislocations (rare) may benefit from open reduction, femoral shortening, varus derotation osteotomy, and Chiari osteotomy;
- VDRO may be successful in 8-10 years olds w/ femoral anteversion and hip dislocation / subluxation;
- late dislocations may best be left out or treated with a Shanz abduction osteotomy;
- windswept hips:
- characterized by abduction of one hip and adduction of contra-lateral hip;
- treatment is best directed at attempting to abduct the adducted hip with bracing or tenotomies;
- scoliosis is treated similarly to idiopathic scoliosis
Current Concepts Review. Management of the Hip in Cerebral Palsy.
The treatment of the painful hip in cerebral palsy by total hip replacement or hip arthrodesis.
Proximal femoral resection to allow adults who have severe cerebral palsy to sit.
Femoral varus-derotation osteotomy in spastic cerebral palsy.
Proximal femoral osteotomy in cerebral palsy.
Pelvic osteotomies for subluxation of the hip in cerebral palsy.
Established hip dislocations in children with cerebral palsy.
Fate of nonoperated hip in cerebral palsy.
Pemberton Pericapsular Osteotomy to treat a dysplastic hip in cerebral palsy.