- Discussion:
- also known as fibrous cortical defect;
- most common bone lesion (40% children);
- it results from defect of periosteal cortical bone development which leads to failure of ossification;
- natural history:
- lesion typically develops in childhood and adolescence;
- during adolescence non ossifying fibroma is an active stage 2 lesion that persists or enlarges throughout childhood.
- w/ skeletal maturation, NOF becomes latent & either regresses or ultimately ossifies;
- when tumor occupies > 50% of diameter of bone, bone is prone to frx;
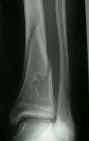
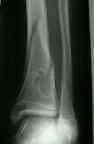
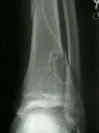
- look for well marginated radiolucent lesion, w/ a distinct multilocular appearance;
- lesion is usually irregular & is surrounded by reactive rim of bone:
- look for benign cortical thinning, erosion, slight expansion;
- there are 2 subtypes;
- fibrous cortical defect;
- more common lesion;
- is small < 0.5 cm radiolucency w/ in cortex w/ sharply defined cortex;
- metaphyseal defect;
- lesion commonly develops in metaphysis of distal femu (90% cases) or the distal tibia & is eccentrically located;
- located within or adjacent to the cortex;
- may be eccentrically located within the medullary cavity;
- cortex may bulge over the lesion, as lack of remodleing;
- may be surrounded by a well defined thin rim of reactive bone;
- no periosteal reaction is seen unless there has been a frx;
- Histology:
- look for whorled fibrous tissue, foam cells, & occasionally, small elongated giant cells;
- diff dx:
- malignant fibrous histiocytoma;
- osteosarcoma;
- histiocytic lymphoma;
- eosinophilic granuloma;
- pyogenic osteomyelitis;
- Frx Management:
- nonossifying fibroma can act as a stress riser in bone which can lead to stress frx w/ heavy running;
- this will result in pain & increase uptake on bone scan;
- in children, closed treatment is the treatment of choice in most cases;
- these fractures fractures are expected to heal with a normal amount of callus, but resolution of the fibroma may or may not occur;
- intracapsular curettage is usually sufficient to promote healing of lesion, however, the defect may be supplemented with bone grafts or
other stabilization techniques for frx prophylaxis and treatment
Benign fibrous histiocytoma of bone
Pathological fractures through non-ossifying fibromas. Review of the Mayo Clinic experience.