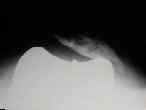
 - See:
- See: - Lateral Retinacular Release:
- Patella in TKR;
- Discussion:
- this is one of the most common causes of failed knee replacement;
- position of each TKR components will determine success of patellar component:
- no patellar prosthesis will track correctly if the components are mal-positioned or if the soft tissues are not balanced;
- often due to malposition of the tibial component;
- patellar symptoms may have nothing to do w/ patellar component other than its reaction with a malrotated femoral or tibial
prosthesis;
- persistent component subluxation or dislocation is usually seen after TKA for severe valgus and external rotation deformities;
- malalignment of the tibial component:
- internal rotation of tibial component is the most frequent cause of tibial femoral malrotation and patellar subluxation;
- position of tibial component can be adjusted to more external rotation, producing relative internal rotation of tibial tubercle,
lessening angle between quadriceps & patellar tendon (Q angle), & thus lessening tendency of the patella to dislocate
laterally;
- if tibial component is inserted w/ tibia externally rotated, patellar ligament will lie laterally to center of prosthetic joint, and the
patella will sublux;
- finally, medialization of the tibial component will increase the Q angle (relative to tibial tubercle) which will also lead to
patellar subluxation;
- femoral component position:
- dislocation may result from internally rotated femoral component (failure to externally rotate 3 deg);
- relative medialization of the femoral component (which increases Q angle);
- insufficient bone resection:
- patella may sublux if insufficient bone has been resected;
- in this case patella is literally lifted out of trochlear groove as knee flexes;
- resecting a portion of patella equal in thickness to patella implant should correct these errors;
- note that the average thickness of the patella in males is 26 mm and in females 24 mm;
- other causes of patellar instability:
- failure to release a tight lateral patellar retinaculum;
- excessive valgus alignment of the knee;
- excessive thickness of the reconstructed patella;
- external rotation of the tibia resulting from implantation of tibial (or femoral) component in internal rotation;
- inadequate centralization of quadriceps muscle force;
- Radiographs:
- lateral subluxation of patella is usually seen on axial view of knee;
- Lateral Retinacular Release:
- if patella still subluxes, then, & only then, should lateral release be performed;
- it is crucial not to perform this lateral release where it is normally performed for lateral subluxation in adolescent;
- it should be performed thru lateral portion of vastus lateralis near its insertion in lateral intermuscular septum;
- this can be done from within the joint and will avoid lateral superior genicular artery;
- take the knee thru a full range of motion several times and check patellar stability;
- lateral patellar subluxation indicates malrotation of the patellar component or, more likely, a contracted lateral retinaculum;
- if lateral retinaculum is contracted, perform lateral retinacular release under direct vision from inside capsule by dividing
synovium, lateral femoropatellar ligament and the lateral retinacular fibers;
- patellar tracking may be improved by removal of patellar osteophytes & lateral retinacular release (and medial reefing);
- Medial Patelloligament Reconstruction:
- medial patellofemoral ligament
- references:
- Medial patellofemoral ligament reconstruction for patellar instability following total knee arthroplasty: A review of 6 cases
- TKR combined with MPLR for OA knee with preoperative valgus deformity and chronic patellar dislocation.
- Medial patellofemoral ligament reconstruction for patellar maltracking following total knee arthroplasty is effective
- Medial patellofemoral ligament reconstruction for recurrent patellar dislocation after total knee arthroplasty
- MPFLR for Patellar Dislocation due to Rupture of the Medial Structures after Total Knee Arthroplasty
- Medial Patellofemoral Ligament Reconstruction Following Total Knee Arthroplasty: A Case Report
- Revision of the Tibial Component:
- position of tibial component can be adjusted to more external rotation, producing relative internal rotation of tibial tubercle,
lessening the angle between quadriceps & patellar tendon, & thus lessening tendency of the patella to dislocate laterally;
- reference:
- Patellar tracking after total knee arthroplasty. The effect of tibial tray malrotation and articular surface configuration.
Patellar tilt and subluxation in total knee arthroplasty. Relationship to pain, fixation, and design.
Patellar dislocation following total knee replacement.
Patellar instability after total knee arthroplasty.
Management of recurrent dislocation of the patella following knee arthroplasty.
A new sugical technique to tibial tubercle transfer in total knee arthroplasty.
The native femoral sulcus as the guide for the medial/lateral position of the femoral component in TKA: Normal patellar tracking in 690/700 knees.
Patellofemoral instability after total knee arthroplasty.
Patellar component stability improves with pulsatile lavage in total knee arthroplasty.
Factors affecting patellar tracking after total knee arthroplasty.
Time dependent changes in patellar tracking with medial parapatellar and midvastus approaches.

