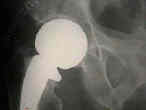
- See: Bipolar Arthroplasty:
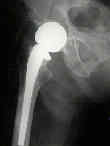
- Discussion:
- indications: indicated for patients w/ a femoral neck frx who meet the following criteria:
- poor general health thay would prevent a second operation;
- pathologic hip fractures:
- parkinson's disease, hemiplegia, or other neurological disease;
- physiologic age > 70 yrs;
- severe osteoporosis w/ loss of primary trabeclae in femoral head (see Sigh Index);
- inadequate closed reduction;
- displaced frx which is several days old;
- pre-existing hip disease (DJD, RA, AVN);
- contraindications:
- preexisting sepsis
- young patient
- failure of internal fixation devices;
- pre-existing dz of the acetabulum;
- even w/ normal preoperative cartilagenous space, many patients will become symptomatic at 5 years due to
metal induced degradation;
- basic science:
- Hemiarthroplasty of hip joint: An experimental validation using porcine acetabulum
- Fluid load support and contact mechanics of hemiarthroplasty in the natural hip joint.
- The response of articular cartilage to weight-bearing against metal. A study of hemiarthroplasty of the hip in the dog
- Effect of hip hemiarthroplasty on articular cartilage and bone in a canine model
- Acetabular involvement in osteonecrosis of the femoral head.
- Degeneration of Acetabular Articular Cartilage to Bipolar Hemiarthroplasty
- Pre Op Planning:
- checklist
- femoral head size:
- if too large, equatorial contact occurs, resulting in a tight joint with a decreased motion and pain;
- if head is too small, polar contact occurs with increased stress over reduced area; leads to erosion, superomedial prosthetic
migration & pain;
- references:
- Hemiarthroplasty of the hip for fracture-What is the appropriate sized femoral head?
- Femoral head measurement in hemiarthroplasty: assessment of interobserver error using 3 measuring systems.
- Degenerative changes in normal femoral heads in the elderly
- Acetabular diameter measurement determines proper prosthetic head size in hemiarthroplasty for femoral head osteonecrosis.
- neck length:
- if the neck is left excessively long, reduction may be difficult and pressure on acetabular cartilage is increased;
- prostheses should be inserted so that the distance between the greater trochanter and center of the femoral head is restored;
- alternatively, attempt to restore the distance between the lesser trochanter and the acetabulum;
- this will restore the length of the abductor mechanism and thereby help to prevent postoperative limp;
- to cement or to not cement ? (cemented femoral stem and cement technique)
- pro-cement argument
- patients w/ a "stove pipe" type of femur (w/ no tapering of medullary canal) are the best candidates for cemented stems,
since there will be a higher risk of fracture with press fit stems in these patients;
- ref: Cemented versus uncemented arthroplasty in patients with a displaced fracture of the femoral neck: a randomised controlled trial.
- risks of cement in hip fractures:
- main risk of cementing is methylmethacrylate embolism (leading to death);
- best ways to avoid cement emobism is thoroughly irrigate the canal and to thoroughly vaccum mix the cement;
- references:
- [Reduction of severe cardiac complications during implantation of cemented total hip endoprostheses in femoral neck fractures].
- Transesophageal echocardiography and clinical features of fat embolism during cemented total hip arthroplasty. A randomized study in patients with a femoral neck fracture.
- Prophylaxis against fat and bone-marrow embolism during total hip arthroplasty reduces the incidence of postoperative deep-vein thrombosis: a controlled, randomized clinical trial.
- Cardiac output during hemiarthroplasty of the hip. A prospective, controlled trial of cemented and uncemented prostheses.
- Lower reoperation rate for cemented hemiarthroplasty than for uncemented hemiarthroplasty and internal fixation following femoral neck fracture: 12- to 19-year follow-up of patients aged 75 years or more.
- Cement emerges as the most predictable option for hip hemiarthroplasty: commentary on an article by Fraser Taylor, BSc, MBChB, FRACS, et al.: "Hemiarthroplasty of the hip with and without cement: a randomized clinical trial".
- pro-press fit argument
- some studies indicate that cemented stems are superior to press fit but the later are often low quality DRG stems (not
plasma spray titanium - see surface coating) - hence comparing apples to oranges;
- note also that many of the premium stems on the market today are blade shaped (which better fit the anatomy of
typical osteoarthritis patient (where as the hip fracture patient will more likely require a more circular "fit and
fill" component (ie one should not pound a trapezoidal component into a circular hole);
- main risk of press fit is periprosthetic fracture;
- if a press fit stem is to be used, then consider using a lateral approach since the fragile osteoporotic bone requires
that the stem be placed in the patients native anteversion (which may or may not provide sufficient stability);
- references:
- Moore hemiarthroplasty with and without bone cement in femoral neck fractures: a clinical controlled trial.
- Treatment of femoral neck fractures with total hip replacement versus cemented and noncemented hemiarthroplasty.
- Hemiarthroplasty of the Hip with and without Cement: A Randomized Clinical Trial
- Is there a difference in perioperative mortality between cemented and uncemented implants in hip fracture surgery?
- Periprosthetic fractures around hip hemiarthroplasty performed for hip fracture.
- Peri-operative mortality after hemiarthroplasty for fracture of the hip: does cement make a difference?
- What should be the preferred choice of hemiarthroplasty technique in American Society of Anesthesiologists (ASA) class III patients with femoral neck fractures? Cemented or cementless.
- Surgical Approaches:
- Anterolateral Approach to Hip Joint: (Watson Jones)
- difficult to perform w/ straight femoral stems, esp if patient is even slightly obese;
- Lateral Approach:
- may be associated w/ limp unless care is taken to minimize dissection of the medius off of the trochanter;
- advantage: is that there is virtually no risk of posterior instability, and therefore, patients do not need hip precautions;
- probably the approach of choice in patients who are demented or who have neurological disorders;
- may be the approach of choice when the stem is to be press fitted since the fragile osteoporotic bone requires that the stem be
placed in patients native anteversion (which may or may not provide sufficient stability);
- Posterior Approach to the Hip Joint
- attempt to re-approximate hip capsule to reduce dislocation;
- note that w/ a displaced femoral neck fracture, the trochanter may be shifted slightly anteriorly, and therefore, consider making
incision slightly more posterior than usual;
- further, it will be easier to broach the femoral canal thru a smaller incision, if the incision is curved more posterior than
usual (towards sciatic notch rather than the PSIS);
- ref: The Moore self locking Vitallium prosthesis in femoral neck frx: a new low posterior approach. AT Moore.
Instr Course Lectures 1959;16:309-321.
- Complications after Hemiarthroplasty:
- mortality:
- Kenzora et. al. 14% mortality during first year after hip frx vs 9% mortality rate in normal population of similar age;
- mortality after hemiarthroplasty is 10 to 40%;
- ref: Outcome after hemiarthroplasty for femoral neck fractures in the elderly
- fracture of the Femur: 4.5%
- almost all frx occur when surgeon attempts to reduce prosthesis;
- most are non displaced and involve either greater troch or neck;
- w/ femoral shaft frx consider methy methacrylate combined w/ a long stem prosthesis;
- dislocation:
- less than 10%.
- more common w/ too much anteversion or retroversion, posterior capuslectomy, & excessive postoperative flexion or rotation
w/ hip adducted;
- reference:
- Botulinum Toxin as a Solution in Voluntary Hip Dislocation After Modular Unipolar Hemiarthroplasty
- post op: sepsis: 2% to 20%
- more common w/ posterior surgical approach;
- infections may be superficial or deep
- ref: Relationship between haematoma in femoral neck fractures contamination and early postop prosthetic joint infection.
- loosening and migration:
- presence of a radiolucent zone around the prosthesis;
- if clinical signs and symptoms are present and loosening or migration is present, then consider revision to THR;
- erosion tends to occur in active pts with cemented Thompson hemiarthroplasty;
- pain:
- painful hemiarthroplasty - conversion to THR
- reference:
- Capsular impingement as a source of pain following bipolar hip arthroplasty.
Clinical and X-ray comparison between a reamed versus an unreamed acetabulum in hip hemiarthroplasty
Thompson hemiarthroplasty and acetabular erosion.
Hemireplacement Arthroplasty with Unipolar vs Bipolar Prosthesis for Displaced Hip Fractures in Elderly
Clinical Results for Bipolar Hemiarthroplasty of the Hip in Patients Under 65 Years Old
Acetabular revision with a bipolar prosthesis.
Rate of degeneration of human acetabular cartilage after hemiarthroplasty.
Bipolar Arthroplasty as a Treatment in Osteoarthritis of the Hip. Preliminary Report
Capsular impingement as a source of pain following bipolar hip arthroplasty.
Bipolar hemiarthroplasty in degenerative arthritis of the hip. 100 consecutive cases.
Precision-fit surface hemiarthroplasty for femoral head osteonecrosis. Long-term results